照顧洗腎的患者時,每個月固定都有很多報告要追蹤解釋,其中,透析前血中尿酸(uric acid)的值,常常需要花一點功夫來解釋,所以,找一些文獻來佐證,充實一下知識。
先找到一篇2004年,台灣臺大與亞東醫院的研究,總共收了146個患者,結果是:太低與太高,死亡率會增加,也就是J-shape(死亡率分布圖,像英文字母 J)的情況。
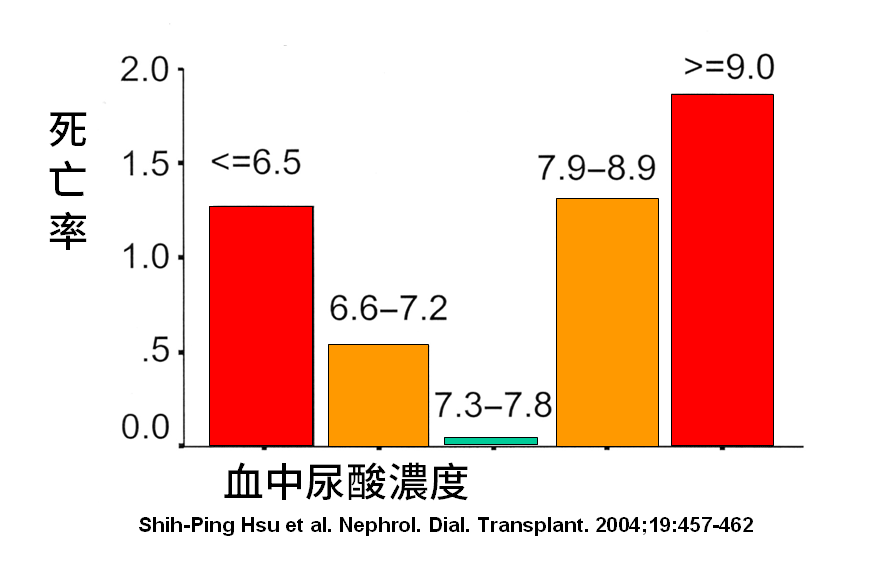
透析患者的報告解讀,往往和正常人不一樣,正常人的尿酸值一般為3-8 mg/dL之間,但從這篇研究可看出,透析患者的尿酸值,即使在正常值內,低於7.2 mg/dL以下,死亡率就開始增加了!這是因為透析患者的尿酸值如果較低,代表營養狀態不夠好,而透析患者的營養狀態,一旦不好,死亡率就上升了。因此,透析前的尿酸值,不能偏低。而這篇研究提到,當尿酸值超過7.9以上,死亡率也會上升,這點和一般正常人相符合。
但是!2011年時,一個歐洲的“大型研究”卻有著不大一樣的結果,一共收了有 4637個患者,結果如下:
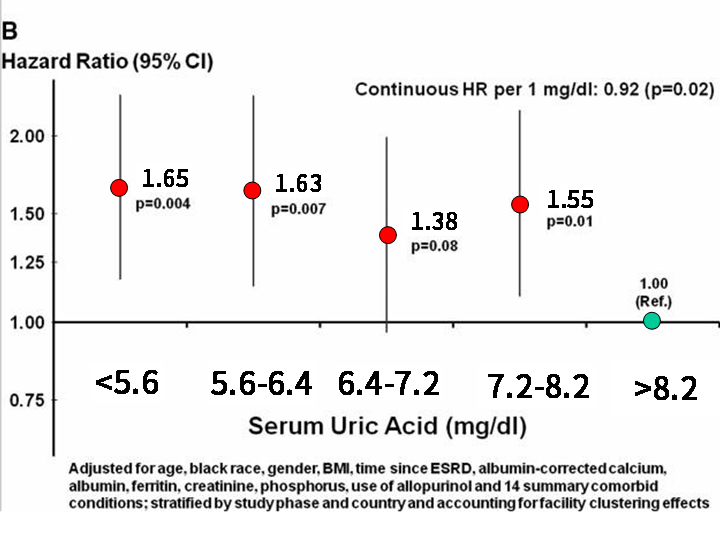
結果這篇研究發現,的確尿酸太低,表示營養差,死亡率會增加沒錯,但是尿酸太高,超過標準值那一組,居然有著最低的死亡率!!這個結果已經校正了很多其他的變數,如:年齡、種族、性別、BMI、白蛋白、血磷值、有無使用降尿酸藥物(allopurinol)等等,結論很簡單:血液透析的患者尿酸值高,死亡率低!
有了血液透析的結果,那麼,腹膜透析呢?這篇2014年中國廣州的研究,直接講結論:對男性患者來說,尿酸越高,總死亡率與心血管疾病死亡率越高;而對女性患者來說,差別不大。
至於,使用降尿酸藥物能不能讓死亡率下降?這篇2014年日本的研究,一共有6252個日本血液透析患者參與,使用allopurinol,對於死亡率的影響,在校正所有變數之後,結果是:沒有太大幫助,只有對於之前沒有發生過心血管疾病的患者,有稍微比較顯著的幫助 (p=0.03)。
總結一下:
1. 血液透析患者血中的尿酸值,高一點應該沒有關係,太低的患者,要注意是否營養不良。
2. 腹膜透析患者血中的尿酸值,男性的尿酸值不能太高,而女性似乎差別不大。
3. 是否使用allopurinal來治療尿酸高,由第一點來看,不大需要,由日本2014年的研究來看,或許沒有發生過心血管疾病的患者,可以考慮使用。
{2147300:69J7PEHF};{2147300:F6JBJS9H};{2147300:35ZX347B};{2147300:5QEJ9DEW}pediatricsdefaultascno638%7B%22status%22%3A%22success%22%2C%22updateneeded%22%3Afalse%2C%22instance%22%3A%22zotpress-ddb9da94181fce1a00c2315e0f270ead%22%2C%22meta%22%3A%7B%22request_last%22%3A0%2C%22request_next%22%3A0%2C%22used_cache%22%3Atrue%7D%2C%22data%22%3A%5B%7B%22key%22%3A%225QEJ9DEW%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Tsuruta%20et%20al.%22%2C%22parsedDate%22%3A%222014%22%2C%22numChildren%22%3A2%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3ETsuruta%20Y%2C%20Nitta%20K%2C%20Akizawa%20T%2C%20et%20al.%20Association%20between%20allopurinol%20and%20mortality%20among%20Japanese%20hemodialysis%20patients%3A%20results%20from%20the%20DOPPS.%20%3Ci%3EInt%20Urol%20Nephrol%3C%5C%2Fi%3E.%202014%3B46%289%29%3A1833-1841.%20%3Ca%20href%3D%27http%3A%5C%2F%5C%2Fdoi.org%5C%2F10.1007%5C%2Fs11255-014-0731-0%27%3Ehttp%3A%5C%2F%5C%2Fdoi.org%5C%2F10.1007%5C%2Fs11255-014-0731-0%3C%5C%2Fa%3E%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Association%20between%20allopurinol%20and%20mortality%20among%20Japanese%20hemodialysis%20patients%3A%20results%20from%20the%20DOPPS%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Yuki%22%2C%22lastName%22%3A%22Tsuruta%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Kosaku%22%2C%22lastName%22%3A%22Nitta%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Tadao%22%2C%22lastName%22%3A%22Akizawa%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Shunichi%22%2C%22lastName%22%3A%22Fukuhara%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Akira%22%2C%22lastName%22%3A%22Saito%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Angelo%22%2C%22lastName%22%3A%22Karaboyas%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Yun%22%2C%22lastName%22%3A%22Li%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Friedrich%20K.%22%2C%22lastName%22%3A%22Port%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Bruce%20M.%22%2C%22lastName%22%3A%22Robinson%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Ronald%20L.%22%2C%22lastName%22%3A%22Pisoni%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Takashi%22%2C%22lastName%22%3A%22Akiba%22%7D%5D%2C%22abstractNote%22%3A%22Purpose%5CnAllopurinol%2C%20for%20treating%20hyperuricemia%2C%20is%20associated%20with%20lower%20mortality%20among%20hyperuricemic%20patients%20without%20chronic%20kidney%20disease%20%28CKD%29.%20Greater%20allopurinol%20utilization%20in%20hemodialysis%20%28HD%29%20in%20Japan%20versus%20other%20countries%20provides%20an%20opportunity%20for%20understanding%20allopurinol-related%20HD%20outcomes.%5Cn%5CnMethods%5CnData%20from%206%2C252%20Japanese%20HD%20patients%20from%20phases%201%5Cu20133%20of%20the%20Dialysis%20Outcomes%20and%20Practice%20Patterns%20Study%20%281999%5Cu20132008%29%20at%20~60%20facilities%20per%20phase%20were%20analyzed.%20Mortality%20was%20compared%20for%20patients%20prescribed%20%2825%5Cu00a0%25%29%20versus%20not-prescribed%20allopurinol%20using%20Cox%20regression%2C%20overall%2C%20and%20in%20patient%20subgroups.%5Cn%5CnResults%5CnPatients%20prescribed%20allopurinol%20were%20more%20likely%20to%20be%20younger%2C%20male%2C%20and%20non-diabetic%2C%20and%20had%20higher%20serum%20creatinine%20and%20lower%20%28treated%29%20serum%20uric%20acid%20levels%20%28mean%5Cu00a0%3D%5Cu00a07.0%20vs.%208.0%5Cu00a0mg%5C%2FdL%2C%20p%5Cu00a0%3C%5Cu00a00.001%29.%20The%20inverse%20association%20between%20allopurinol%20prescription%20and%20mortality%20in%20unadjusted%20analyses%20%28HR%200.65%2C%2095%5Cu00a0%25%20CI%200.52%5Cu20130.81%29%20was%20attenuated%20by%20covariate%20adjustment%20%28HR%200.84%2C%200.66%5Cu20131.06%29.%20In%20subgroup%20analyses%2C%20allopurinol%20was%20associated%20with%20lower%20mortality%20among%20patients%20with%20no%20history%20of%20cardiovascular%20disease%20%28CVD%29%20%28HR%200.48%2C%200.28%5Cu20130.83%29%2C%20but%20not%20among%20patients%20with%20CVD%20%28HR%201.00%2C%200.76%5Cu20131.32%29.%20A%20similar%20pattern%20was%20seen%20outside%20Japan%20and%20for%20cardiovascular%20%28CV%29-related%20mortality.%5Cn%5CnConclusions%5CnAllopurinol%20prescription%20was%20not%20significantly%20associated%20with%20case-mix-adjusted%20mortality%20in%20Japanese%20HD%20patients%20overall%2C%20but%20was%20associated%20with%20lower%20all-cause%20and%20CV-related%20mortality%20in%20the%20subgroup%20of%20patients%20with%20no%20prior%20CVD%20history.%20These%20findings%20in%20HD%20patients%20may%20be%20related%20to%20findings%20in%20non-dialysis%20CKD%20patients%20showing%20lower%20CV%20event%20rates%20and%20mortality%2C%20and%20improved%20endothelial%20function%20with%20allopurinol%20prescription.%20These%20results%20are%20useful%20for%20designing%20future%20trials%20of%20allopurinol%20use%20in%20HD%20patients.%22%2C%22date%22%3A%222014%22%2C%22language%22%3A%22%22%2C%22DOI%22%3A%2210.1007%5C%2Fs11255-014-0731-0%22%2C%22ISSN%22%3A%220301-1623%22%2C%22url%22%3A%22http%3A%5C%2F%5C%2Fwww.ncbi.nlm.nih.gov%5C%2Fpmc%5C%2Farticles%5C%2FPMC4147244%5C%2F%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-03-27T12%3A52%3A54Z%22%7D%7D%2C%7B%22key%22%3A%2235ZX347B%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Xia%20et%20al.%22%2C%22parsedDate%22%3A%222014-08%22%2C%22numChildren%22%3A1%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3EXia%20X%2C%20He%20F%2C%20Wu%20X%2C%20Peng%20F%2C%20Huang%20F%2C%20Yu%20X.%20Relationship%20between%20serum%20uric%20acid%20and%20all-cause%20and%20cardiovascular%20mortality%20in%20patients%20treated%20with%20peritoneal%20dialysis.%20%3Ci%3EAm%20J%20Kidney%20Dis%3C%5C%2Fi%3E.%202014%3B64%282%29%3A257-264.%20%3Ca%20href%3D%27http%3A%5C%2F%5C%2Fdoi.org%5C%2F10.1053%5C%2Fj.ajkd.2013.08.027%27%3Ehttp%3A%5C%2F%5C%2Fdoi.org%5C%2F10.1053%5C%2Fj.ajkd.2013.08.027%3C%5C%2Fa%3E%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Relationship%20between%20serum%20uric%20acid%20and%20all-cause%20and%20cardiovascular%20mortality%20in%20patients%20treated%20with%20peritoneal%20dialysis%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Xi%22%2C%22lastName%22%3A%22Xia%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Feng%22%2C%22lastName%22%3A%22He%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Xianfeng%22%2C%22lastName%22%3A%22Wu%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Fenfen%22%2C%22lastName%22%3A%22Peng%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Fengxian%22%2C%22lastName%22%3A%22Huang%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Xueqing%22%2C%22lastName%22%3A%22Yu%22%7D%5D%2C%22abstractNote%22%3A%22BACKGROUND%3A%20Although%20serum%20uric%20acid%20level%20appears%20to%20be%20associated%20with%20mortality%20in%20individuals%20treated%20with%20hemodialysis%2C%20the%20relationship%20between%20serum%20uric%20acid%20level%20and%20death%20is%20uncertain%20in%20patients%20treated%20with%20peritoneal%20dialysis%20%28PD%29.%5CnSTUDY%20DESIGN%3A%20Cohort%20study.%5CnSETTING%20%26%20PARTICIPANTS%3A%20985%20patients%20from%20a%20single%20PD%20center%20in%20South%20China%20followed%20up%20for%20a%20median%20of%2025.3%20months.%5CnPREDICTOR%3A%20Serum%20uric%20acid%20level.%5CnOUTCOMES%20%26%20MEASUREMENTS%3A%20The%20association%20of%20baseline%20sex-specific%20uric%20acid%20level%20with%20all-cause%20and%20cardiovascular%20mortality%20was%20evaluated.%20Models%20were%20adjusted%20for%20age%2C%20body%20mass%20index%2C%20comorbidity%20score%2C%20residual%20kidney%20function%2C%20total%20Kt%5C%2FV%2C%20allopurinol%20and%20angiotensin-converting%20enzyme%20inhibitor%5C%2Fangiotensin%20receptor%20blocker%20use%2C%20and%20laboratory%20test%20results%2C%20including%20hemoglobin%2C%20serum%20albumin%2C%20creatinine%2C%20calcium%2C%20phosphorus%2C%20triglycerides%2C%20low-density%20lipoprotein%20cholesterol%2C%20and%20high-sensitivity%20C-reactive%20protein.%5CnRESULTS%3A%20Mean%20age%20was%2048.3%5Cu00b115.4%20%28SD%29%20years%2C%20and%2023%25%20had%20diabetes.%20Mean%20uric%20acid%20level%20was%207.0%5Cu00b11.3%20%28range%2C%203.8-19.8%29%20mg%5C%2FdL.%20During%20follow-up%2C%20144%20deaths%20were%20recorded%2C%20of%20which%2064%20were%20due%20to%20cardiovascular%20events.%20In%20multivariable%20models%2C%20the%20highest%20sex-specific%20tertile%20of%20uric%20acid%20level%20was%20associated%20with%20increased%20risk%20of%20all-cause%20mortality%20%28HR%2C%201.93%3B%2095%25%20CI%2C%201.27-2.93%3B%20P%3D0.004%29%20and%20cardiovascular%20mortality%20%28HR%2C%203.31%3B%2095%25%20CI%2C%201.70-6.41%3B%20P%3C0.001%29%20compared%20to%20the%20lowest%20tertile.%20Adjusted%20Cox%20regression%20models%20showed%20that%20the%20HRs%20per%201-mg%5C%2FdL%20higher%20uric%20acid%20level%20for%20all-cause%20and%20cardiovascular%20mortality%20were%201.33%20%2895%25%20CI%2C%201.14-1.56%3B%20P%3C0.001%29%20and%201.44%20%2895%25%20CI%2C%201.17-1.77%3B%20P%3D0.001%29%20for%20men%20and%201.03%20%2895%25%20CI%2C%200.86-1.24%3B%20P%3D0.8%29%20and%201.16%20%2895%25%20CI%2C%200.97-1.38%3B%20P%3D0.1%29%20for%20women%2C%20respectively.%20A%20formal%20test%20for%20interaction%20indicated%20that%20the%20association%20of%20uric%20acid%20level%20with%20all-cause%20and%20cardiovascular%20mortality%20differed%20by%20sex%20%28%5Cu03b2%20%3D%20-0.06%20%5BP%3D0.02%5D%20and%20%5Cu03b2%20%3D%20-0.10%20%5BP%3D0.02%5D%2C%20respectively%29.%5CnLIMITATIONS%3A%20Single%20measurement%20of%20uric%20acid%20at%20baseline.%20Cause%20of%20death%20determined%20by%20death%20certificates%20and%20expert%20consensus.%5CnCONCLUSIONS%3A%20Elevated%20serum%20uric%20acid%20level%20is%20an%20independent%20risk%20factor%20for%20all-cause%20and%20cardiovascular%20mortality%20in%20men%20treated%20with%20PD.%22%2C%22date%22%3A%22Aug%202014%22%2C%22language%22%3A%22eng%22%2C%22DOI%22%3A%2210.1053%5C%2Fj.ajkd.2013.08.027%22%2C%22ISSN%22%3A%221523-6838%22%2C%22url%22%3A%22%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-03-27T12%3A45%3A17Z%22%7D%7D%2C%7B%22key%22%3A%22F6JBJS9H%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Latif%20et%20al.%22%2C%22parsedDate%22%3A%222011-10%22%2C%22numChildren%22%3A1%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3ELatif%20W%2C%20Karaboyas%20A%2C%20Tong%20L%2C%20et%20al.%20Uric%20Acid%20Levels%20and%20All-Cause%20and%20Cardiovascular%20Mortality%20in%20the%20Hemodialysis%20Population.%20%3Ci%3EClin%20J%20Am%20Soc%20Nephrol%3C%5C%2Fi%3E.%202011%3B6%2810%29%3A2470-2477.%20%3Ca%20href%3D%27http%3A%5C%2F%5C%2Fdoi.org%5C%2F10.2215%5C%2FCJN.00670111%27%3Ehttp%3A%5C%2F%5C%2Fdoi.org%5C%2F10.2215%5C%2FCJN.00670111%3C%5C%2Fa%3E%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Uric%20Acid%20Levels%20and%20All-Cause%20and%20Cardiovascular%20Mortality%20in%20the%20Hemodialysis%20Population%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Walead%22%2C%22lastName%22%3A%22Latif%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Angelo%22%2C%22lastName%22%3A%22Karaboyas%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Lin%22%2C%22lastName%22%3A%22Tong%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22James%20F.%22%2C%22lastName%22%3A%22Winchester%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Charlotte%20J.%22%2C%22lastName%22%3A%22Arrington%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Ronald%20L.%22%2C%22lastName%22%3A%22Pisoni%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Mark%20R.%22%2C%22lastName%22%3A%22Marshall%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Werner%22%2C%22lastName%22%3A%22Kleophas%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Nathan%20W.%22%2C%22lastName%22%3A%22Levin%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Ananda%22%2C%22lastName%22%3A%22Sen%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Bruce%20M.%22%2C%22lastName%22%3A%22Robinson%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Rajiv%22%2C%22lastName%22%3A%22Saran%22%7D%5D%2C%22abstractNote%22%3A%22Summary%5Cnnull%22%2C%22date%22%3A%222011-10%22%2C%22language%22%3A%22%22%2C%22DOI%22%3A%2210.2215%5C%2FCJN.00670111%22%2C%22ISSN%22%3A%221555-9041%22%2C%22url%22%3A%22http%3A%5C%2F%5C%2Fwww.ncbi.nlm.nih.gov%5C%2Fpmc%5C%2Farticles%5C%2FPMC3359562%5C%2F%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-03-27T12%3A22%3A42Z%22%7D%7D%2C%7B%22key%22%3A%2269J7PEHF%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Shih-Ping%20Hsu%22%2C%22parsedDate%22%3A%222004%22%2C%22numChildren%22%3A1%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3EShih-Ping%20Hsu%20MFP.%20Serum%20uric%20acid%20levels%20show%20a%20%26amp%3B%2339%3BJ-shaped%26amp%3B%2339%3B%20association%20with%20all-cause%20mortality%20in%20haemodialysis%20patients.%20%3Ci%3ENephrology%2C%20dialysis%2C%20transplantation%26%23x202F%3B%3A%20official%20publication%20of%20the%20European%20Dialysis%20and%20Transplant%20Association%20-%20European%20Renal%20Association%3C%5C%2Fi%3E.%202004%3B19%282%29%3A457-462.%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Serum%20uric%20acid%20levels%20show%20a%20%26%2339%3BJ-shaped%26%2339%3B%20association%20with%20all-cause%20mortality%20in%20haemodialysis%20patients.%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Mei-Fen%20Pai%22%2C%22lastName%22%3A%22Shih-Ping%20Hsu%22%7D%5D%2C%22abstractNote%22%3A%22%22%2C%22date%22%3A%222004%22%2C%22language%22%3A%22%22%2C%22DOI%22%3A%22%22%2C%22ISSN%22%3A%220931-0509%22%2C%22url%22%3A%22%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-03-27T12%3A22%3A33Z%22%7D%7D%5D%7D 1.
Tsuruta Y, Nitta K, Akizawa T, et al. Association between allopurinol and mortality among Japanese hemodialysis patients: results from the DOPPS.
Int Urol Nephrol. 2014;46(9):1833-1841.
http://doi.org/10.1007/s11255-014-0731-0 1.
Xia X, He F, Wu X, Peng F, Huang F, Yu X. Relationship between serum uric acid and all-cause and cardiovascular mortality in patients treated with peritoneal dialysis.
Am J Kidney Dis. 2014;64(2):257-264.
http://doi.org/10.1053/j.ajkd.2013.08.027 1.
Latif W, Karaboyas A, Tong L, et al. Uric Acid Levels and All-Cause and Cardiovascular Mortality in the Hemodialysis Population.
Clin J Am Soc Nephrol. 2011;6(10):2470-2477.
http://doi.org/10.2215/CJN.00670111 1.
Shih-Ping Hsu MFP. Serum uric acid levels show a 'J-shaped' association with all-cause mortality in haemodialysis patients. Nephrology, dialysis, transplantation : official publication of the European Dialysis and Transplant Association - European Renal Association. 2004;19(2):457-462.





