上一篇提到,透析液鈣離子(Ca)的建議濃度約在Ca=2.5-3.0 meq/L,而或許2.5 meq/L(以下關於濃度的敘述,都是指透析液鈣離子濃度)是目前最接近的好答案,但是應該視患者之情況來做出調整,而非一體適用。
這些建議確實留下了一堆問號,或許2013年的這篇研究,能夠讓未來的透析治療更精緻化。
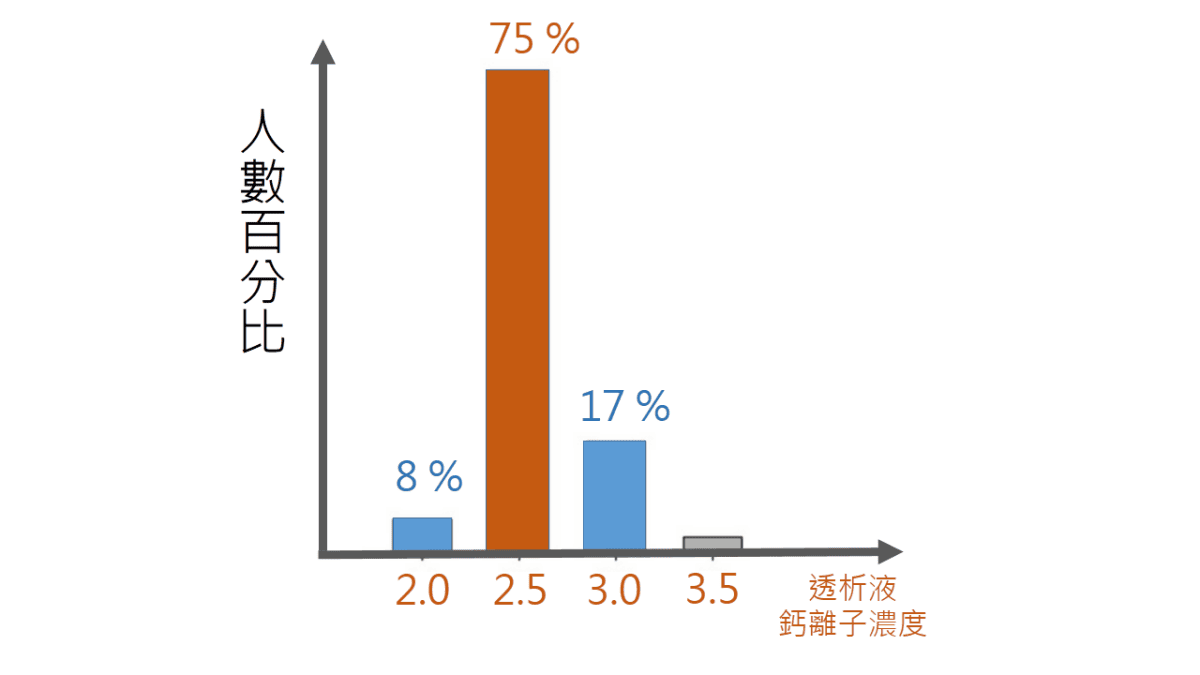
先看看人家大多使用哪種透析液吧!從圖中可看得出來,75%的患者,都使用2.5 meq/L的透析液。

這篇研究結果指出,使用 2.0 meq/L濃度以下的透析液、或患者血中校正後鈣離子濃度較高,都會增加突發性心臟停止(sudden cardiac arrest)的機會。事實上,這篇研究的亮點是,透析液的鈣離子,與血液中的鈣離子,若濃度差異太大,也會增加突發性心臟停止的危險性,濃度差異每增加 1 meq/L,危險性變為1.4倍。[OR: 1.40 (95% CI: 1.10–1.80) p= 0.002 ]
這篇研究令人恍然大悟啊。
雖然透析是在有限的時間內,矯正身體裡多餘的水分與毒素廢物,但是我們都知道,要如何讓患者洗的平穩舒服,其實大方向很明確,就是讓患者在透析過程中,體內的變化盡可能越小越好,不管是毒素的變化、或水分的變化(請參考:脫水速度有沒有上限?)。看起來,鈣離子的變化幅度是否太大,也是需要注意的。
而透析液鈣離子濃度,也是有個下限的,如果用濃度小於 2.0 meq/L的透析液,突發性心臟停止的危險性,將變為兩倍。[OR: 2.00 (95% CI: 1.40–2.90) p<0.001 ]。仔細看內文,那些使用2.0 meq/L的患者,他們血中鈣離子濃度都超過 10 mg/dL,這表示,如果為了降血鈣,而選用2.0 meq/L的透析液,反而會使得血液與透析液的鈣離子濃度差異太大,容易導致危險。
那麼,臨床醫師如果真的遇到血鈣很高,又想要在透析的時候,幫患者多降一點鈣離子,選用2.5 meq/L的透析液,到底能夠洗出多少鈣呢?在後續的雜誌編輯討論中,也提到另一篇研究,能夠解答這個問題,這篇研究提到,當患者的PTH <300 pg/ml時,使用2.5 meq/L的透析液,可以透析出347 mg (± 605)的鈣,而如果是PTH>300 pg/ml者,則可以透析出 626 mg (± 487) 的鈣。
因此,本篇重點結錄:
1. 使用 2.5 meq/L的透析液,確實能夠幫助身體除去多餘的鈣離子,而又不會增加危險性。
2. 絕大部分的患者,都是使用 2.5 meq/L的透析液的,這是為了不讓鈣離子累積在身體中,為了血管的健康。
請與照顧您的醫師,討論透析液鈣離子濃度,盡可能讓身體減少鈣離子的負擔吧!
{2147300:CTHQ48EP};{2147300:DXFC9JI4};{2147300:SCT5IE5N}pediatricsdefaultascno742%7B%22status%22%3A%22success%22%2C%22updateneeded%22%3Afalse%2C%22instance%22%3A%22zotpress-f5db665aedf64a95805a95723e947bcd%22%2C%22meta%22%3A%7B%22request_last%22%3A0%2C%22request_next%22%3A0%2C%22used_cache%22%3Atrue%7D%2C%22data%22%3A%5B%7B%22key%22%3A%22SCT5IE5N%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Karohl%20et%20al.%22%2C%22parsedDate%22%3A%222010-04-01%22%2C%22numChildren%22%3A3%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3EKarohl%20C%2C%20Paschoal%20J%20de%20P%2C%20Castro%20MCM%20de%2C%20et%20al.%20Effects%20of%20bone%20remodelling%20on%20calcium%20mass%20transfer%20during%20haemodialysis.%20%3Ci%3ENephrol%20Dial%20Transplant%3C%5C%2Fi%3E.%202010%3B25%284%29%3A1244-1251.%20%3Ca%20href%3D%27http%3A%5C%2F%5C%2Fdoi.org%5C%2F10.1093%5C%2Fndt%5C%2Fgfp597%27%3Ehttp%3A%5C%2F%5C%2Fdoi.org%5C%2F10.1093%5C%2Fndt%5C%2Fgfp597%3C%5C%2Fa%3E%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Effects%20of%20bone%20remodelling%20on%20calcium%20mass%20transfer%20during%20haemodialysis%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Cristina%22%2C%22lastName%22%3A%22Karohl%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Juliana%20de%20Paiva%22%2C%22lastName%22%3A%22Paschoal%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Manuel%20Carlos%20Martins%20de%22%2C%22lastName%22%3A%22Castro%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Rosilene%20Motta%22%2C%22lastName%22%3A%22Elias%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Hugo%22%2C%22lastName%22%3A%22Abensur%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Jo%5Cu00e3o%20Eg%5Cu00eddio%22%2C%22lastName%22%3A%22Rom%5Cu00e3o%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Jutta%22%2C%22lastName%22%3A%22Passlick-Deetjen%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Vanda%22%2C%22lastName%22%3A%22Jorgetti%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Rosa%20Maria%20Affonso%22%2C%22lastName%22%3A%22Moys%5Cu00e9s%22%7D%5D%2C%22abstractNote%22%3A%22Background.%20During%20haemodialysis%2C%20calcium%20balance%20can%20affect%2C%20or%20be%20affected%20by%2C%20mineral%20metabolism.%20However%2C%20when%20dialysate%20calcium%20concentration%20%28d%5BCa%5D%29%20is%20chosen%20or%20kinetic%20models%20are%20employed%20to%20calculate%20calcium%20balance%2C%20bone%20remodelling%20is%20rarely%20considered.%20In%20this%20study%2C%20we%20examined%20whether%20bone%20remodelling%20affects%20calcium%20mass%20transfer%20during%20haemodialysis.%5CnMethods.%20We%20dialysed%2023%20patients%20using%20a%20d%5BCa%5D%20of%201.0%2C%201.25%2C%201.5%20or%201.75%20mmol%5C%2FL.%20Calcium%20mass%20transfer%20was%20measured%20and%20associated%20with%20remodelling%20bone%20factors.%5CnResults.%20Calcium%20balance%20varied%20widely%20depending%20on%20the%20d%5BCa%5D.%20Calcium%20removal%20was%20%5Cu2212578%20%5Cu00b1%20389%2C%20%5Cu2212468%20%5Cu00b1%20563%2C%20%2B46%20%5Cu00b1%20400%20and%20%2B405%20%5Cu00b1%20413%20mg%20when%20a%20d%5BCa%5D%20of%201.0%2C%201.25%2C%201.5%20or%201.75%20mmol%5C%2FL%20was%20used%2C%20respectively%20%281.0%20and%201.25%20vs%201.5%20and%201.75%20mmol%5C%2FL%2C%20P%20%3C%200.001%3B%201.5%20vs%201.75%20mmol%5C%2FL%2C%20P%20%3C%200.05%29.%20Univariate%20analysis%20showed%20that%20calcium%20balance%20correlated%20with%20calcium%20gradient%2C%20parathyroid%20hormone%20%28PTH%29%2C%20osteocalcin%20and%20dialysis%20vintage.%20Multivariate%20analysis%20revealed%20that%20calcium%20balance%20was%20dependent%20on%20calcium%20gradient%2C%20PTH%20and%20osteocalcin.%5CnConclusions.%20These%20results%20suggest%20that%20bone%20remodelling%20could%20affect%20calcium%20mass%20transfer%20during%20haemodialysis.%22%2C%22date%22%3A%2204%5C%2F01%5C%2F2010%22%2C%22language%22%3A%22en%22%2C%22DOI%22%3A%2210.1093%5C%2Fndt%5C%2Fgfp597%22%2C%22ISSN%22%3A%220931-0509%2C%201460-2385%22%2C%22url%22%3A%22http%3A%5C%2F%5C%2Fndt.oxfordjournals.org%5C%2Fcontent%5C%2F25%5C%2F4%5C%2F1244%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-04-07T03%3A16%3A03Z%22%7D%7D%2C%7B%22key%22%3A%22CTHQ48EP%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Pun%20et%20al.%22%2C%22parsedDate%22%3A%222013-05%22%2C%22numChildren%22%3A1%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3EPun%20PH%2C%20Horton%20JR%2C%20Middleton%20JP.%20Dialysate%20calcium%20concentration%20and%20the%20risk%20of%20sudden%20cardiac%20arrest%20in%20hemodialysis%20patients.%20%3Ci%3EClin%20J%20Am%20Soc%20Nephrol%3C%5C%2Fi%3E.%202013%3B8%285%29%3A797-803.%20%3Ca%20href%3D%27http%3A%5C%2F%5C%2Fdoi.org%5C%2F10.2215%5C%2FCJN.10000912%27%3Ehttp%3A%5C%2F%5C%2Fdoi.org%5C%2F10.2215%5C%2FCJN.10000912%3C%5C%2Fa%3E%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Dialysate%20calcium%20concentration%20and%20the%20risk%20of%20sudden%20cardiac%20arrest%20in%20hemodialysis%20patients%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Patrick%20H.%22%2C%22lastName%22%3A%22Pun%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22John%20R.%22%2C%22lastName%22%3A%22Horton%22%7D%2C%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22John%20P.%22%2C%22lastName%22%3A%22Middleton%22%7D%5D%2C%22abstractNote%22%3A%22BACKGROUND%20AND%20OBJECTIVES%3A%20The%20optimal%20dialysate%20calcium%20concentration%20to%20maintain%20normal%20mineralization%20and%20reduce%20risk%20of%20cardiovascular%20events%20in%20hemodialysis%20patients%20is%20debated.%20Guidelines%20suggest%20that%20dialysate%20Ca%20concentration%20should%20be%20lowered%20to%20avoid%20vascular%20calcification%2C%20but%20cardiac%20arrhythmias%20may%20be%20more%20likely%20to%20occur%20at%20lower%20dialysate%20Ca.%20Concurrent%20use%20of%20QT-prolonging%20medications%20may%20also%20exacerbate%20arrhythmic%20risk.%20This%20study%20examined%20the%20influence%20of%20serum%20Ca%2C%20dialysate%20Ca%2C%20and%20QT%20interval-prolonging%20medications%20on%20the%20risk%20of%20sudden%20cardiac%20arrest%20in%20a%20cohort%20of%20hemodialysis%20patients.%5CnDESIGN%2C%20SETTING%2C%20PARTICIPANTS%2C%20%26%20MEASUREMENTS%3A%20This%20case-control%20study%20among%2043%2C200%20hemodialysis%20patients%20occurred%20between%202002%20and%202005%3B%20510%20patients%20who%20experienced%20a%20witnessed%20sudden%20cardiac%20arrest%20were%20compared%20with%201560%20matched%20controls.%20This%20study%20examined%20covariate-adjusted%20sudden%20cardiac%20arrest%20risk%20associations%20with%20serum%20Ca%2C%20dialysate%20Ca%2C%20serum%20dialysate%20Ca%20gradient%2C%20and%20prescription%20of%20QT-prolonging%20medications%20using%20logistic%20regression%20techniques.%5CnRESULTS%3A%20Patients%20assigned%20to%20low%20Ca%20dialysate%3C2.5%20mEq%5C%2FL%20were%20more%20likely%20to%20be%20exposed%20to%20larger%20serum%20dialysate%20Ca%20gradient%20and%20had%20a%20greater%20fall%20in%20BP%20during%20dialysis%20treatment.%20After%20accounting%20for%20covariates%20and%20baseline%20differences%2C%20low%20Ca%20dialysate%3C2.5%20mEq%5C%2FL%20%28odds%20ratio%3D2.00%2C%2095%25%20confidence%20interval%3D1.40-2.90%29%2C%20higher%20corrected%20serum%20Ca%20%28odds%20ratio%3D1.10%2C%2095%25%20confidence%20interval%3D1.00-1.30%29%2C%20and%20increasing%20serum%20dialysate%20Ca%20gradient%20%28odds%20ratio%3D1.40%2C%2095%25%20confidence%20interval%3D1.10-1.80%29%20were%20associated%20with%20increased%20risk%20of%20sudden%20cardiac%20arrest%2C%20whereas%20there%20were%20no%20significant%20risk%20associations%20with%20QT-prolonging%20medications.%5CnCONCLUSIONS%3A%20Increased%20risk%20of%20sudden%20cardiac%20arrest%20associated%20with%20low%20Ca%20dialysate%20and%20large%20serum%20dialysate%20Ca%20gradients%20should%20be%20considered%20in%20determining%20the%20optimal%20dialysate%20Ca%20prescription.%22%2C%22date%22%3A%22May%202013%22%2C%22language%22%3A%22eng%22%2C%22DOI%22%3A%2210.2215%5C%2FCJN.10000912%22%2C%22ISSN%22%3A%221555-905X%22%2C%22url%22%3A%22%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-04-03T09%3A15%3A21Z%22%7D%7D%2C%7B%22key%22%3A%22DXFC9JI4%22%2C%22library%22%3A%7B%22id%22%3A2147300%7D%2C%22meta%22%3A%7B%22creatorSummary%22%3A%22Bleyer%22%2C%22parsedDate%22%3A%222013-05-07%22%2C%22numChildren%22%3A3%7D%2C%22bib%22%3A%22%3Cdiv%20class%3D%5C%22csl-bib-body%5C%22%20style%3D%5C%22line-height%3A%201.35%3B%20%5C%22%3E%5Cn%20%20%3Cdiv%20class%3D%5C%22csl-entry%5C%22%20style%3D%5C%22clear%3A%20left%3B%20%5C%22%3E%5Cn%20%20%20%20%3Cdiv%20class%3D%5C%22csl-left-margin%5C%22%20style%3D%5C%22float%3A%20left%3B%20padding-right%3A%200.5em%3B%20text-align%3A%20right%3B%20width%3A%201em%3B%5C%22%3E1.%20%3C%5C%2Fdiv%3E%3Cdiv%20class%3D%5C%22csl-right-inline%5C%22%20style%3D%5C%22margin%3A%200%20.4em%200%201.5em%3B%5C%22%3EBleyer%20AJ.%20Clinical%20Implications%20of%20the%20Relationship%20between%20Low%20Calcium%20Concentration%20Dialysate%20and%20Sudden%20Death.%20%3Ci%3ECJASN%3C%5C%2Fi%3E.%202013%3B8%285%29%3A706-707.%20%3Ca%20href%3D%27http%3A%5C%2F%5C%2Fdoi.org%5C%2F10.2215%5C%2FCJN.03130313%27%3Ehttp%3A%5C%2F%5C%2Fdoi.org%5C%2F10.2215%5C%2FCJN.03130313%3C%5C%2Fa%3E%3C%5C%2Fdiv%3E%5Cn%20%20%3C%5C%2Fdiv%3E%5Cn%3C%5C%2Fdiv%3E%22%2C%22data%22%3A%7B%22itemType%22%3A%22journalArticle%22%2C%22title%22%3A%22Clinical%20Implications%20of%20the%20Relationship%20between%20Low%20Calcium%20Concentration%20Dialysate%20and%20Sudden%20Death%22%2C%22creators%22%3A%5B%7B%22creatorType%22%3A%22author%22%2C%22firstName%22%3A%22Anthony%20J.%22%2C%22lastName%22%3A%22Bleyer%22%7D%5D%2C%22abstractNote%22%3A%22%22%2C%22date%22%3A%2205%5C%2F07%5C%2F2013%22%2C%22language%22%3A%22en%22%2C%22DOI%22%3A%2210.2215%5C%2FCJN.03130313%22%2C%22ISSN%22%3A%221555-9041%2C%201555-905X%22%2C%22url%22%3A%22http%3A%5C%2F%5C%2Fcjasn.asnjournals.org%5C%2Fcontent%5C%2F8%5C%2F5%5C%2F706%22%2C%22collections%22%3A%5B%5D%2C%22dateModified%22%3A%222015-04-03T07%3A48%3A23Z%22%7D%7D%5D%7D 1.
Karohl C, Paschoal J de P, Castro MCM de, et al. Effects of bone remodelling on calcium mass transfer during haemodialysis.
Nephrol Dial Transplant. 2010;25(4):1244-1251.
http://doi.org/10.1093/ndt/gfp597 1.
Pun PH, Horton JR, Middleton JP. Dialysate calcium concentration and the risk of sudden cardiac arrest in hemodialysis patients.
Clin J Am Soc Nephrol. 2013;8(5):797-803.
http://doi.org/10.2215/CJN.10000912 1.
Bleyer AJ. Clinical Implications of the Relationship between Low Calcium Concentration Dialysate and Sudden Death.
CJASN. 2013;8(5):706-707.
http://doi.org/10.2215/CJN.03130313